Introduction: Why Ringworm vs Eczema Matters
Red, itchy patches on the skin can be alarming, but confusion between ringworm and eczema is common—and potentially costly. Misidentifying these two conditions might delay the right treatment or even worsen symptoms. This article aims to demystify the differences between ringworm and eczema, outlining clear symptoms, causes, and diagnostic strategies, so you can take the right steps for healthier skin and peace of mind.
Understanding Ringworm vs Eczema: Definitions, Scope, and Relevance
Distinguishing ringworm from eczema is crucial for tailoring effective treatment and avoiding complications. Both present as skin rashes but are fundamentally different.
Ringworm (dermatophytosis) is a highly contagious fungal infection characterized by circular, red, scaly patches with a clear edge. Despite its name, no worms are involved; the “ring” refers to its shape. Eczema, formally known as atopic dermatitis, is an inflammatory, non-infectious skin condition. It produces dry, itchy, sometimes blistering areas that often lack a clear border. Knowing whether you have ringworm or eczema guides both treatment and prevention.
Why Accurate Identification Matters
For patients and caregivers, a correct diagnosis ensures timely relief and prevents unnecessary suffering. Treating ringworm as eczema (or vice versa) can lead to complications: antifungal medications are ineffective against eczema, and steroid creams may aggravate fungal infections. Efficient and accurate differentiation leads to quicker healing and reduces transmission risk in community settings.
Core Approach to Distinguishing and Treating Ringworm vs Eczema
Successful management begins with a systematic assessment of symptoms, risk factors, and targeted treatment.
Recognize the Distinctive Symptoms
- Ringworm: Look for red or pink, ring-shaped lesions with a scaly, raised border and clearer center. Commonly appears on the scalp, body, feet (athlete’s foot), or groin (jock itch). May be mildly to severely itchy.
- Eczema: Typically manifests as persistently dry, itchy, inflamed patches. Lacks a clear border; skin may become thickened and cracked from chronic scratching. Frequently affects folds of the limbs, neck, and face, especially in children.
Diagnostic Checks
- Medical History: Ringworm is often contracted from direct contact with infected people, animals, or surfaces. Eczema tends to run in families with allergies or asthma.
- Physical Examination: Dermatologists examine lesion shape, location, and secondary signs (like crusting or blistering).
- Laboratory Testing: For ambiguous cases, skin scrapings from the lesion can be examined under a microscope or cultured to detect fungus.
Treatment Decision Criteria
- Ringworm: Requires antifungal creams or oral medications, depending on severity and site.
- Eczema: Managed primarily with moisturizers, topical corticosteroids, and avoidance of triggers. Severe cases may benefit from immune-modulating drugs.
Monitoring Progress
- Improvement for both conditions is expected within 1–3 weeks after starting correct therapy. Lack of progress warrants reevaluation—especially to rule out misdiagnosis.
Tools and Metrics to Guide Management
Accurate and ongoing assessment is vital for optimal outcomes.
- Symptom Tracker: Maintain a diary noting size, intensity, and number of lesions.
- Itch and Pain Scales: Rate discomfort daily to monitor response to treatment.
- Photography: Take weekly pictures to objectively assess changes, as skin rashes can subtly shift.
Data and Proof: Prevalence and Treatment Insights
Key Statistics
- Atopic dermatitis (eczema) affects about 10% of adults and up to 20% of children globally (World Allergy Organization, 2022).
- About 20–25% of fungal skin infections are caused by dermatophytes, responsible for most cases of ringworm (CDC, 2021).
What Do These Numbers Mean?
For the average patient, these statistics reveal how common and easily confused these skin issues are. A vast number of people wrestle with diagnosis each year, underscoring the importance of distinguishing and treating the right condition promptly, especially since ringworm is contagious and eczema, though not, often recurs or persists.
Practical Examples: Real-World Scenarios
Example A: Distinct Path, Clear Outcome
A 9-year-old boy develops a circular, itchy rash on his arm after playing with a neighbor’s cat. The pediatrician notes a defined, raised border and recommends a KOH test, which reveals fungal elements. Antifungal cream is prescribed; within two weeks, symptoms resolve completely. Early identification of ringworm prevented its spread to other family members.
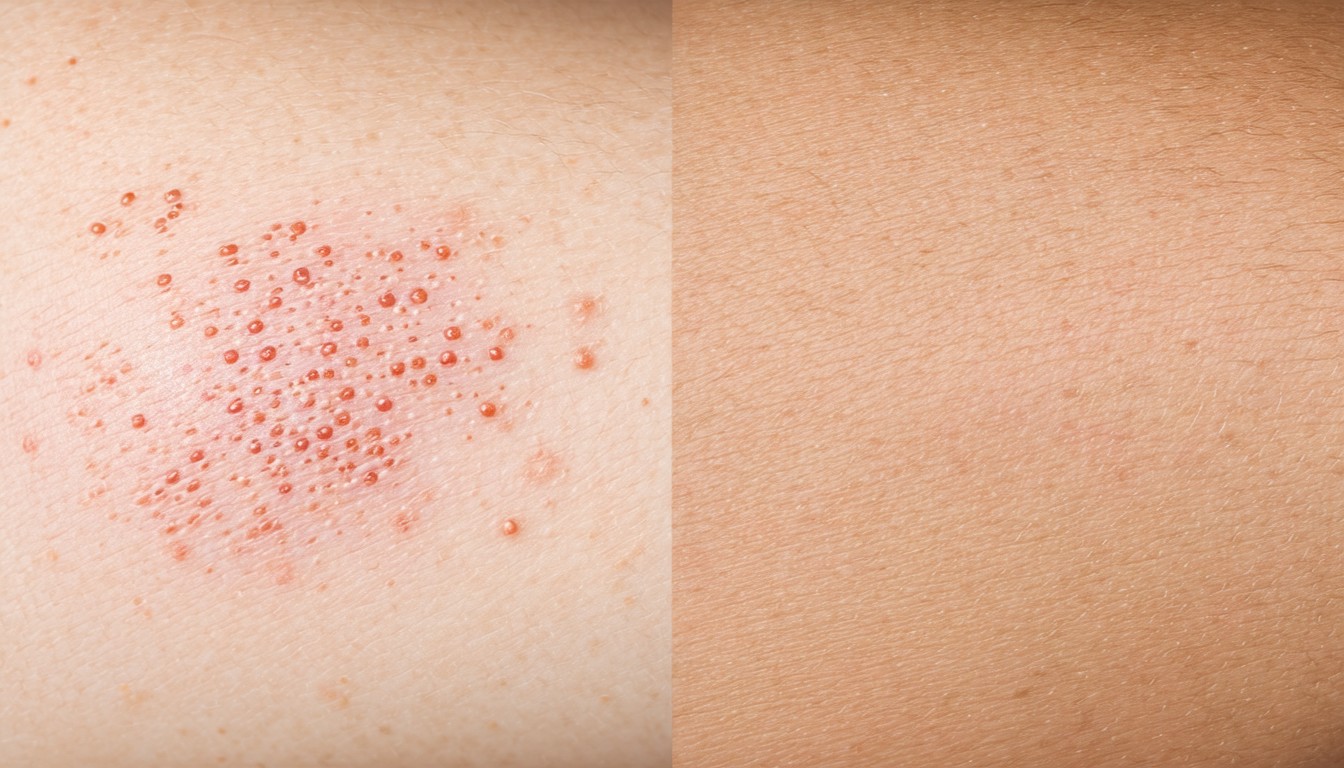
Example B: The Consequence of Mistaken Identity
A working adult woman notices dry, itchy patches on her elbows and uses a friend’s leftover antifungal lotion with no relief. Her rash worsens over months. On seeing a dermatologist, she is diagnosed with eczema—with a family history of allergies—and prescribed topical steroids and moisturizers. Her symptoms clear within days, highlighting the cost in time and discomfort when ringworm and eczema are confused.
Avoiding Common Mistakes
Missteps in diagnosis and management are frequent but preventable:
- Applying Steroids to Ringworm: This can mask symptoms and promote fungus growth, making infections harder to treat.
- Overuse of Antifungals for Eczema: Wastes time and money, prolonging discomfort.
- Neglecting Triggers in Eczema: Failing to address allergens or irritants can cause repeated flare-ups.
- Ignoring Household Contamination for Ringworm: Fomites (towels, bedding) can harbor the fungus—cleanliness matters.
Myth-busting: Despite folklore, neither condition reflects poor hygiene—ringworm is spread by contact, and eczema is linked to genetics and environment.
Implementation Checklist
- Examine rash carefully for shape, border, and texture.
- Consider exposure history: contact with infected people/animals (ringworm), allergies or family history (eczema).
- Avoid self-diagnosis with over-the-counter creams before a clear diagnosis.
- Seek medical evaluation for persistent or unclear rashes.
- Begin prescribed treatment diligently and monitor progress.
- Practice good hygiene for ringworm; moisturize and protect skin for eczema.
- Reassess or consult a dermatologist if symptoms do not improve within 2–3 weeks.
Conclusion: Key Takeaways and Next Steps
Differentiating ringworm vs eczema is essential for choosing effective treatment and regaining comfort. While both conditions cause skin irritation, their causes, treatments, and risks differ sharply. Recognizing symptom patterns, seeking timely diagnosis, and following targeted treatments can prevent complications and speed recovery. If you notice a rash that is not responding to basic self-care, prioritize a medical evaluation—correct identification leads to the relief you need.
FAQs
How can I tell if a rash is ringworm or eczema?
Ringworm usually appears as a red, circular patch with a clearer center and raised border, while eczema looks more like dry, patchy areas without defined edges. A medical evaluation is recommended for a definitive diagnosis.
What happens if I treat eczema with antifungals or ringworm with steroids?
Misusing these treatments may make the condition worse—steroids can mask ringworm and encourage its spread, while antifungals have no effect on eczema. It is best to confirm your diagnosis before starting any medication.
Is either ringworm or eczema contagious?
Ringworm is highly contagious through skin-to-skin contact and contaminated objects. Eczema is not contagious and results from genetic and environmental factors.
When should I see a doctor about skin rashes like ringworm or eczema?
If a rash lasts more than two weeks, worsens, or does not respond to basic care, consult a healthcare provider. Painful, spreading, or infected-looking rashes require prompt attention.
Are there ways to prevent ringworm and eczema outbreaks?
Ringworm prevention hinges on hygiene, avoiding contact with infected persons or animals, and disinfecting common surfaces. Eczema flare-ups are minimized by moisturizing regularly and avoiding personal triggers like harsh soaps or allergens.
Can children get both ringworm and eczema at the same time?
Yes, it is possible, especially as both conditions are common in children. If symptoms are complex or persistent, seek a healthcare professional for thorough assessment.



